Physical exercises are known to improve the quality of life. When you exercise, you reduce the chances of getting heart diseases; you loose weight or perhaps maintain a healthy weight and you become physically fit. Here are the main benefits of exercise for patients with type 1 diabetes:




While you exercise, you are using a lot of your muscles that require more energy compared to non active muscles, as a result more glucose leaves your blood and gets into your muscles causing a drop in your blood sugar. The amount of insulin you take before exercising can be another cause, if you took your insulin without eating and then started to exercise, your blood sugar may drop quickly because insulin itself reduces your blood sugar and while exercising your blood sugar will normally drops so combining those factors causes further drop in your blood sugar.
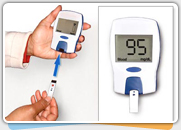

Yes, a drop in your blood sugar may occur during exercise or delayed up to 24-36 hours after exercising.


"Check your blood sugar before, during, and after the exercise" that’s the golden role for making sure that you wont undergo hypoglycemia due to exercising. Record your blood sugar readings, this will allow you to adjust your need of either an additional snack or insulin dose requirement ( consult your physician about your pre-exercise insulin dose). Always include in your record the following:
These records can be very helpful to your physician/ dietitian as she or he will have a guide in how to control your blood sugar.
If you are going to exercise around mealtime, you should eat the meal first. Try to begin the exercise 30 to 60 minutes after a meal or snack. Keep in mind those points when you are having your pre-exercise meal or snack:
If your blood sugar is less than 100 mg/dL (5.5 mmol/L) eat a carbohydrate snack (at least 15 grams of carb) before you exercise. check your blood sugar 15 to 30 minutes later. Do not exercise until your blood sugar is higher than 100 mg/dL (5.5 mmol/L).
You should always have a source of sugar available.
The type of a needed snack varies depending on the type and the expected duration of the exercise, for example:
It is very useful to monitor your blood sugar to figure out what the correct type and amount of snack you may need.
|
The rate of insulin absorption during exercise is very much related to the site of insulin injection. Since blood flow increases in the body parts that are moving during activity, the absorption of insulin injected into this part increases. Avoid injecting the body parts that you are going to use during exercise, for example: do not inject insulin into your leg if you are going to run, or avoid injecting your arm that you will be using for playing squash. The abdomen is usually a good injection site before exercising.


You need to follow the regular protocol when you experience hypoglycemia, blood sugar less than 70 mg/dL (3.8 mmol/L) . Follow the rule of 15 which is 15 grams of carbohydrates, measure blood sugar after 15 minutes. Examples of 15 grams of carbs include.
check your blood glucose again after 15 minutes, If it’s still too low, have another serving. Repeat until your blood glucose is 70 mg/dL (3.8 mmol/L) or higher. If it will be an hour or more before your next meal, have a snack that consists of complex carbohydrates; such as cheese sandwich.
Yes, you may talk to your doctor about that, he/she will reduce your insulin dose according to the readings of your blood sugar before, during, and after exercising. Reducing your dose will avoid the drop of your blood sugar without the need for additional intake of carbohydrates.


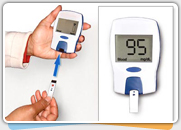

It is always better to measure your blood sugar before, during and immediately after exercise and at 4-5 hours after exercise just to make sure that things are going well. If you are a beginner, you may need to measure your blood sugar every 15 minutes and less often if you are a participant. If you always do the same type of exercise with the same duration and all your readings are normal, then you don’t have to measure that often unless you changed the type of exercise or the duration.


Yes, blood sugar may increase during/after exercise, especially for those who choose to do high-intensity exercise. When people (with or without diabetes) intensely exercise, or be under the stress of competition or even under excessive heat, some hormones get released into their blood that causes an increase in blood sugar. In people without diabetes, this increase in blood sugar is not noticeable because their pancreas can release adequate amount of insulin that will normalize blood sugar, but for you, since the pancreas is incapable of producing insulin your blood sugar remains high after exercising.
Taking a low dose of insulin before exercising could also be another reason for getting high blood sugar during exercise. Consult your doctor if you think that your pre-exercise insulin dose is not enough.


If your blood sugar always increases during exercise, you may consult your doctor and ask him/her to adjust your pre-exercise dose. Remember to bring your blood sugar readings before, during and after exercising so the doctor can adjust your dose accordingly. In addition, try to drink enough amount of water after exercising; you can also drink a little water every half an hour during your exercise (*)
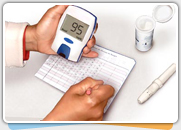

Yes, since weight lifting is considered to be a high-intensity exercise, it can increase your blood sugar dramatically. If you are an athlete with diabetes, weight lifting performed until exhaustion often elevates your blood sugar after exercise. You can use a correction dose after exercising depending on your blood sugar readings. Ask your doctor or diabetes dietitian about correcting your dose.


Yes, you should not exercise when your blood sugar is
Keep up on our always evolving product features and technology. Enter your e-mail and subscribe to our newsletter.